How to Recognize and Treat the Less Well-Known Silent Heart Killer Afflicting Six Million People
How to Recognize and Treat the Less Well-Known Silent Heart Killer Afflicting Six Million People
If you mention the words “silent killer” to many lay people and doctors, most would answer coronary heart disease (CAD), commonly known as the hardening of the arteries. Indeed CAD can cause heart attacks, sudden cardiac death, and lethal heart irregularities in people with no symptoms. However, it is less well appreciated that one-third of people with atrial fibrillation (AF) may also have no symptoms, and not knowing may have lethal consequences.
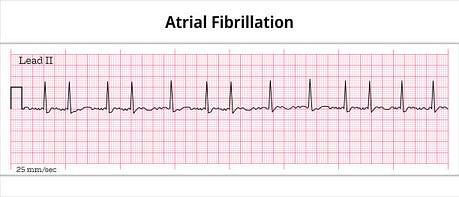
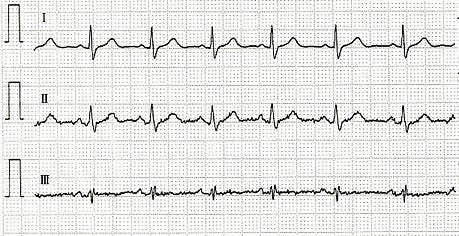
AF is usually a rapid, irregular heartbeat. Please take a look at the above photo of an electrocardiogram. Now contrast that with the photo below, which shows a normal, slower, regular beat-to-beat heart rhythm again on an electrocardiogram.
One study examined the risks of dying if you have AF within one year. They found the risk was ten percent or one out of ten people. To understand the risks, you must first understand the difference between AF and a more lethal form of rapid heart irregularity, ventricular fibrillation (VF). A quick anatomy lesson is worthwhile in this regard.
There are four human heart chambers: two upper ones, named atria, and two lower ones, named ventricles. Each category also has two on the right and left sides of the body. The ventricles are responsible for pumping blood to the lungs and the rest of the body. Upon receiving blood from the body’s veins, the atria hold blood and dump it into the ventricles every 50–100 times per minute. The 50–100 times is equivalent to our pulse or heart rate.
The heart muscle in both the atria and ventricle knows when to beat after receiving an electrical signal from specialized cells in the heart muscle. It is like being stimulated with a mini-cattle prod. A tiny electric shock causes muscles to jump. An electrocardiogram (ECG or EKG) can record this electrical signal. Rapid and irregular heart rhythms can arise from the atria (AF) or the ventricles (VF). VF is immediately lethal, and AF is not.
This distinction is important because no one usually dies from AF itself. Rather, if left untreated, the rapid and irregular nature of AF causes blood to thicken and form clots in the atria since the chambers are quivering and not opening and closing regularly. Thus, blood tends to pool or sit inside. Then, pieces of the clot break off and may cause strokes, many of which are lethal. Thus, the consequences of AF, not AF itself, can kill you.
But how can it be detected if one-third of patients don’t even know they have it? An EKG, of course, can identify it, but most of us don’t commonly get this more than once a year and often far less frequently. You could learn to check your pulse to see if it is irregular. It is not hard to learn.
You can also can get a home blood pressure (BP) machine that will automatically read your BP and pulse rate. Many people with hypertension or high BP have or should own one. They can be purchased for under $40. Any interaction with dental or healthcare professionals should include a routine screening and pulse check. They are also readily available for free in most drug stores.
Ways that people with AF die
I have already described one common scenario where the consequences of untreated AF may kill you. That is a stroke. Some diseases make AF more common. And these diseases can kill you, too. Those are hypertension, sleep apnea, diabetes, CAD, valvular heart disease, diabetes, advanced age, male gender, obesity, overactive thyroid, and heart failure. Treating the underlying disease(s) will often help treat the AF.
Treatments options
The first is to identify if the AF is present. An EKG is confirmatory or a monitor that you can wear from a doctor. Garmin and Apple offer two popular hardware and apps that accomplish this.
Ideally, you should see a cardiologist to rule in or out other causes of the AF. One easily treatable cause is excess alcohol. Too much alcohol, in any form, can cause AF even without other diseases and a normal heart. As a practicing cardiologist, I saw this frequently around holidays. Cardiologists and the emergency room docs labeled it “holiday heart syndrome.”
Whether or not the AF is a one-time occurrence without heart disease, so-called “lone AF” or episodic or chronic dictates the treatment options. Again, a cardiology consult is helpful, and often the patient will be referred to an Electrophysiologist (EP), a cardiologist specializing in disorders of the heart rhythm.
Many patients will be placed on blood thinners to prevent lethal blood clots from forming. If the heart rate is rapid with the AF, medications to slow the heart rate might also be prescribed. Medications might also be prescribed to keep patients out of AF and in normal rhythm. All medications come with side effects, some of them serious. Thus, competent medical advice is necessary.
If all else fails, the EP doctor can perform a radio-frequency catheter ablation (RFA) procedure by inserting a tube into the heart under X-Ray guidance to “zap” the areas causing the heart to fibrillate. Although RFA carries a low risk, there is a tendency for the AF to recur, and it is not uncommon to need a second and even third procedure.
There is an old medical axiom: “An ounce of prevention is worth a pound of cure.” It has merit, and when dealing with AF, the earlier it can be identified and treated, the less likely AF is to kill you.